Jo Harris
RCVS Recognised Specialist in Cardiology
The dyspnoeic cat is a fairly common presentation in first-opinion practice, and it is easy to underestimate how fragile and critical these patients are. It is vital to recognise dyspnoea and act swiftly, from phone triage through to diagnostic approach in the clinic.
Most cats find car journeys stressful, and hence any cat in respiratory distress should be placed in an oxygen-rich environment (be mindful that small oxygen tents can get very hot and humid) or given free-flow oxygen supplementation, whilst a brief history is collected. Observation of respiratory pattern and a brief clinical examination can give important clues as to the underlying disease:
- Inspiratory effort (especially with audible stridor) usually indicates upper respiratory tract obstruction e.g. foreign body or laryngeal paralysis
- Hyperpnoea is a slower, deep breathing pattern, often described as paradoxical due to use of abdominal muscles to increase the effort. This is common in cats with pleural effusions but may also indicate diaphragmatic rupture following trauma.
- Fast shallow breathing is typical of pulmonary oedema, but other lung disease can give a similar pattern. Differential diagnoses include feline asthma, bronchopneumonia or trauma causing pulmonary contusions or rib damage.
Clinical examination
Unfortunately in cats, single clinical findings are not particularly useful in reaching a diagnosis. For example tachycardia and pulmonary crackles are common with stress and a variety of lung disease. Heart murmurs are common in cats both with and without heart disease, although gallop sounds and arrhythmias are more commonly associated with cardiac disease.
In cats presenting with acute respiratory distress without obvious signs of trauma, a simple algorithm involving a combination of a simple TPR (rectal temperature, heart rate and respiratory rate) and cardiac auscultation has been shown to give an accurate indication of presence of cardiac vs non-cardiac dyspnoea (the RAPID CAT study, Dickson et al, 2018). This does not give a definitive diagnosis but helps to guide emergency therapy until further diagnostic tests can be safely achieved:
- Temp < 37.5C
- Heart rate > 200bpm
- Resp rate > 75 br/min
This combination of findings is highly specific for presence of cardiac dyspnoea – meaning that acute congestive heart failure is extremely likely. A gallop sound on auscultation is also highly suggestive of cardiac dyspnoea.
The RAPID CAT algorithm is not particularly sensitive, meaning not all findings are present in all cardiac patients. But if all these are present, and/or a gallop sound is identified, you can start diuretic therapy with reasonable confidence until the patient is stable enough for further tests.
NT-proBNP SNAP test
This simple bedside blood test, available from IDEXX, tests for presence of myocardial stretch, and is useful in rapid assessment of dyspnoeic cats. This is a highly sensitive screening test, meaning that almost all cats with true underlying cardiac disease should be detected (although false positives are common).
The important take-home message is that a negative test gives reasonable confidence that the cat is not suffering from acute congestive heart failure, and feline asthma or other causes are more likely. A positive test means cardiac disease may well be present; starting furosemide is a reasonable course of action, but further tests are needed to be sure.
Ultrasound scan
Learning to perform a focused thoracic ultrasound scan or “TFAST” is extremely useful. This can be performed with the cat in sternal recumbency receiving oxygen therapy, and in cases of pleural effusion or obvious left atrial enlargement gives an immediate diagnosis for the
cause of dyspnoea:
 |
 |
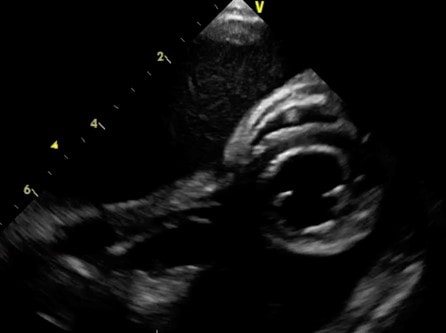
| Black anechoic space surrounding the heart in a cat with pleural effusion |
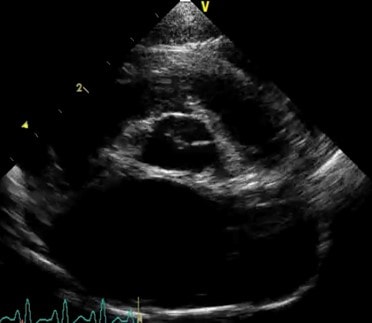
Left atrial enlargement in a cat with acute CHF |
Lung ultrasound is an emerging technique which can help to differentiate between normal lung tissue, interstitial infiltration (such as oedema, pneumonia) and pneumothorax as well as identifying consolidation, masses or pyothorax/pleural effusion. The technique is best learnt with formal training and requires practice to be useful in reliable and repeatable rapid assessment of patients.
Radiography
Radiographing dyspnoeic cats is best avoided due to the obvious stress involved in restraint. If this is your only option, then placing the cat in sternal recumbency with no restraint, or in a cat carrier surrounded by foam pads is the safest technique.
Radiographs from dyspnoeic cats can be very difficult to interpret, but findings associated with congestive heart failure in cats include:
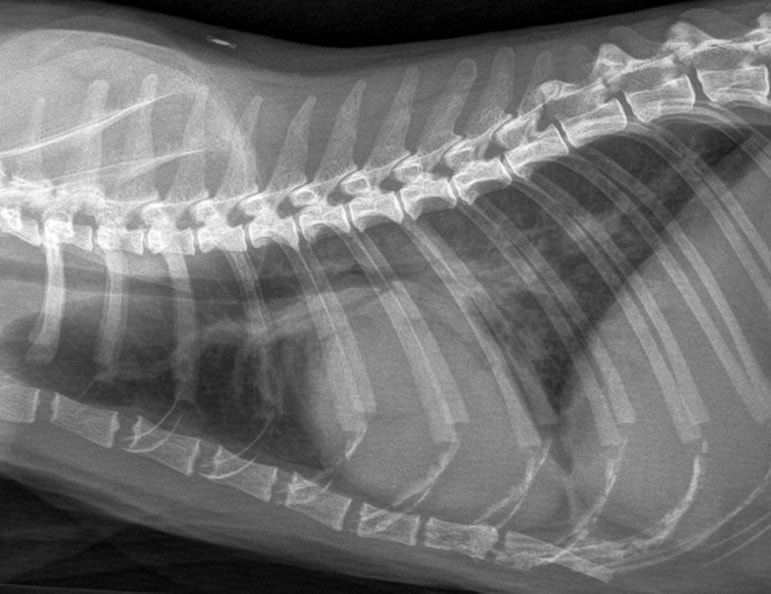
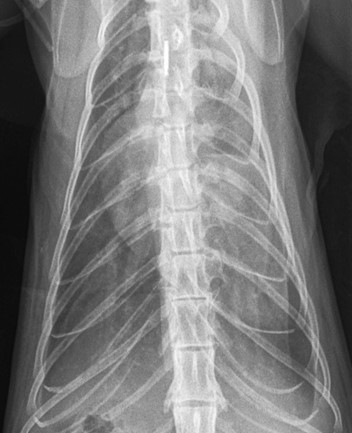
- Left atrial enlargement – a “kidney bean” shape on the lateral view or “valentine” shape on the DV (note this is not always particularly obvious, and many cats do not have generalised cardiomegaly).
- Congestion of pulmonary lobar vessels – often most prominent on the DV view. These are unlikely to be even visible in cats with other causes of a visible lung pattern
- Patchy interstitial/alveolar lung pattern associated with pulmonary oedema – often spreading from the region of the pulmonary vessels but can be very variable in cats.
 |
 |
Treatment
Treatment depends on the underlying disease and hence there is no “one size fits all” treatment for dyspnoeic cats. Some useful tips include:
- DO avoid stress and minimise handling. Very anxious or fractious patients may benefit from a low dose of butorphanol sedation (0.2mg/kg IM)
- DO supplement oxygen
- DO NOT try blind thoracocentesis – even the most novice sonographer can safely pop an ultrasound probe on the chest to look for pleural effusion.
- DO try to learn to estimate left atrial size in a conscious cat – left atrial enlargement is key to diagnosing CHF with certainty.
- If a pleural effusion is identified then thoracocentesis should be performed immediately, ideally, ultrasound-guided.
- Cats with pulmonary oedema should be treated with furosemide I/V (if a catheter can be placed safely) or I/M at 1-2mg/kg initial dose, followed by 1mg/kg hourly until respiratory rate is 40 breaths/min or less.
- A one-off dose of furosemide whilst performing diagnostic tests is unlikely to do harm, and may be life-saving. However remember this is also bronchodilator in most species and may appear to give some improvement in asthmatic cats too. Any improvement should not be taken as a diagnosis – further tests are still necessary to make an accurate diagnosis and make an ongoing treatment plan.



